 I’ve been in physical therapy since October. First it was for my leg/ankle, which were broken last July. Having spent three months with no weight-bearing on the right leg, I needed a lot of help getting back to walking.
I’ve been in physical therapy since October. First it was for my leg/ankle, which were broken last July. Having spent three months with no weight-bearing on the right leg, I needed a lot of help getting back to walking.
In January I did a few weeks of P.T. for my neck, which was also broken last July. My pain level in my neck and shoulders is pretty manageable most days, although my range of motion is limited.
On January 29 I started a third round of P.T. This time it’s for my right hip/gluts. Evidently I aggravated this area during the months I was lying in bed with external fixation (metal rods) sticking out of my leg, and later with a cast. I hopped around on one leg for a few months, and when I began walking, I limped.
 So here I am, almost eight months since my wreck and surgeries, and I’m in pain. Every day. Almost every step I take. Sometimes it wakes me up at night. This weekend my husband and I went for a couple of long walks here in our beautiful neighborhood on the Mississippi River. The weather was gorgeous, and it lifted our spirits greatly. But every step I took sent pain through my hip and buttocks. And later my ankle also started hurting.
So here I am, almost eight months since my wreck and surgeries, and I’m in pain. Every day. Almost every step I take. Sometimes it wakes me up at night. This weekend my husband and I went for a couple of long walks here in our beautiful neighborhood on the Mississippi River. The weather was gorgeous, and it lifted our spirits greatly. But every step I took sent pain through my hip and buttocks. And later my ankle also started hurting.
I haven’t taken any pain meds since last July, and I don’t plan to. I want to learn to manage this with physical therapy, massage therapy, heat and ice, stretching and strengthening exercises, and rest. But it sure does wear on me, mentally and emotionally, at times. So I decided to do a little reading about chronic pain. Here are two links, in case any of you are also dealing with this:
How to Cope With Chronic Pain offers some good advice. Click on the link to read more about:
Accepting the pain.
Keeping a pain journal.
Talking about it.
Getting your grief out.
Being mindful of what helps and what hurts.
A good point in this second article is that there is a difference in pain and suffering:
The experience of the pain can either be one of suffering (“this is unbearable”) or one of tolerance and existence (“my pain slows me down but I won’t let it stop me”). The difference is a state of mind, not a state of physical injury. Physical limits exist, but how people face them is a choice.
This was helpful to me, so I read further in the same article:
In addition, a person’s personality traits, social supports, life history, substance use, spiritual perspective and life stressors all impact the level of pain experienced—your reaction to difficult circumstances can be changed, with help.
 A third article discusses the relationship between pain and depression:
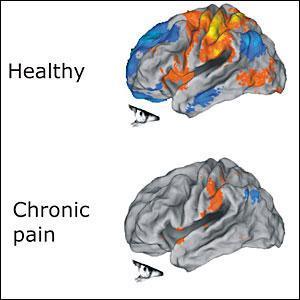
A third article discusses the relationship between pain and depression:
When pain lasts longer than a few weeks, areas of the spinal cord change their physiology, and ‘learn’ to maintain the pain, even if you don’t want it. Similarly, long-standing depression changes your brain, reducing the amount of grey matter in important regions. Depression can be the result of pain, and pain can be the result of depression.
So, as I continue to do whatever I can do help minimize the pain, I’m also going to try to react to it differently. Distractions help, and I’ve got plenty of them to keep my mind of the pain as much as possible—helping my husband as he continues to recover from rotator cuff surgery (11 days ago), preparing for a visit from my daughter and granddaughter (in two weeks), and preparing for our MOVE, in 40 days! But even in my caregiving, grandmothering, and move organizing, I know I need to pace myself in order to manage the pain. I just remembered that my “One Word” for 2014 is mindfulness.

This is very helpful, Susan. The hardest thing for me has been to talk about the pain the arthritis in my hips causes. I will try to be more honest about it – thanks for sharing these resources.
I tend to err in the other direction, Ellen… to talk too much about the pain. So that really isn’t my “weakness” in all this. But learning the difference in pain and suffering intrigues me. Thanks, always, for reading and commenting.
2 things that stand out for me in this- the idea of acceptance- I would like to know more about the slow steps you are taking towards that, I am fascinated by that. And pain management without the medications. I see on FB that you are using a combo acupressure and Eft… Non- pharmacological techniques would go far in reducing our Opiod addiction problem. It’s good to know what else to recommend to patients. Thanks! Brave lady!
Hi, Nina. I haven’t started doing anything with the “tapping” yet. Just heard about it yesterday. I’m going to watch a few more videos about it and decide whether it’s something I can try on my own. If it’s not too difficult to find the places to “tap” on my body, I think it’s worth a try. And yes, taking slow steps towards acceptance is a challenge, but one I’m making, since I don’t know how much of this pain I will be living with once my body has done all the healing it can do. I’m real sensitive to meds, which is why I only used the pain meds for a couple of weeks after the initial surgery. And of course I didn’t want to have an addition issue.